Markets Confusing? Ask Edgen Search.
Instant answers, zero BS, and trading decisions your future self will thank you for.
Análisis de acciones de UnitedHealth Group: La potencia de la integración vertical en salud | Edgen

Resumen
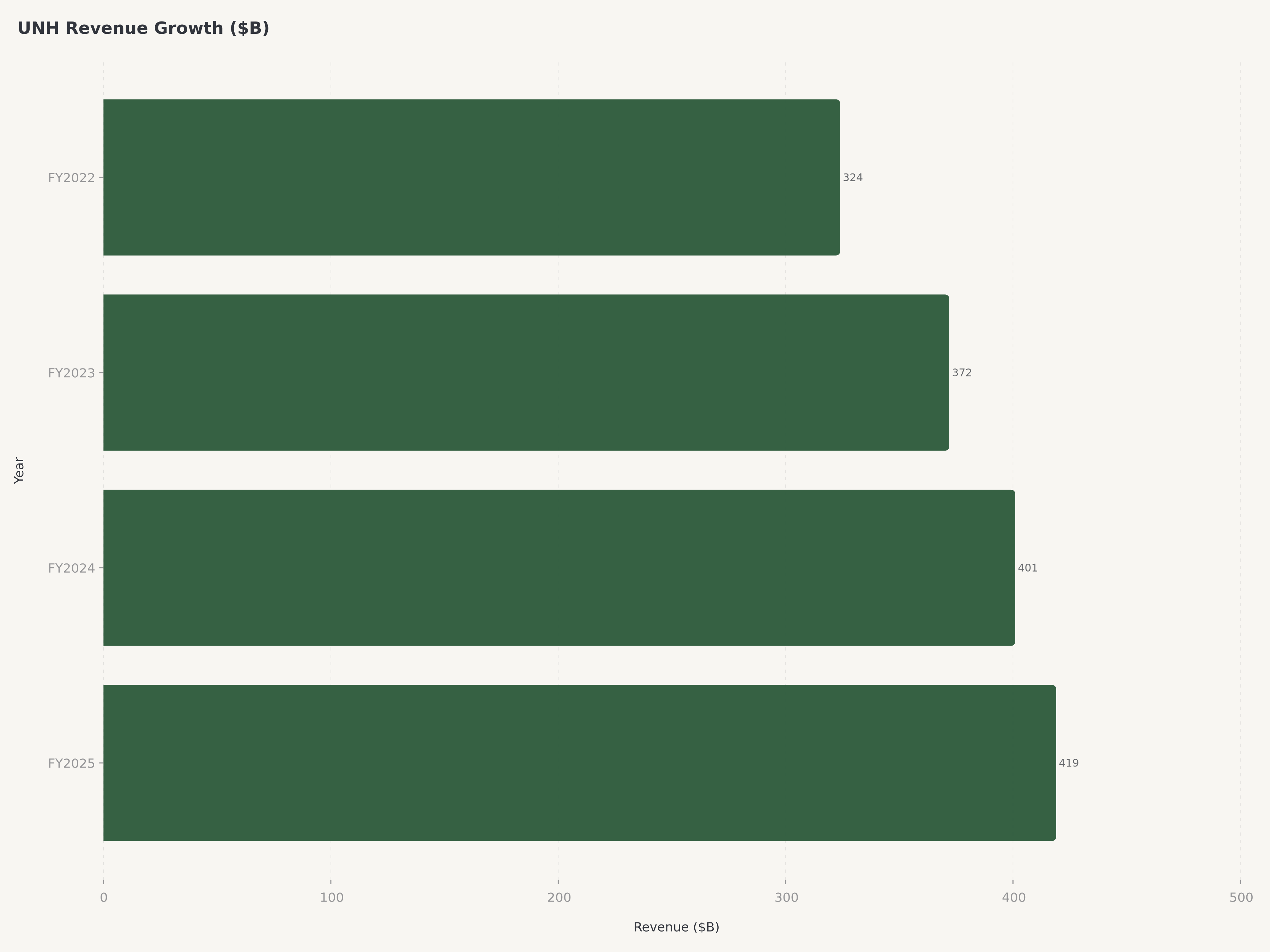
- Ingresos y escala: Los ingresos del año fiscal 2025 alcanzaron los 419.300 millones de dólares (+12% interanual), consolidando a UnitedHealth Group como la empresa más grande por ingresos en el sistema de salud de EE. UU. La plataforma Optum —que abarca servicios de salud, tecnología y beneficios farmacéuticos— se ha convertido en el principal motor de crecimiento, con Optum Rx registrando la expansión más rápida en toda la empresa.
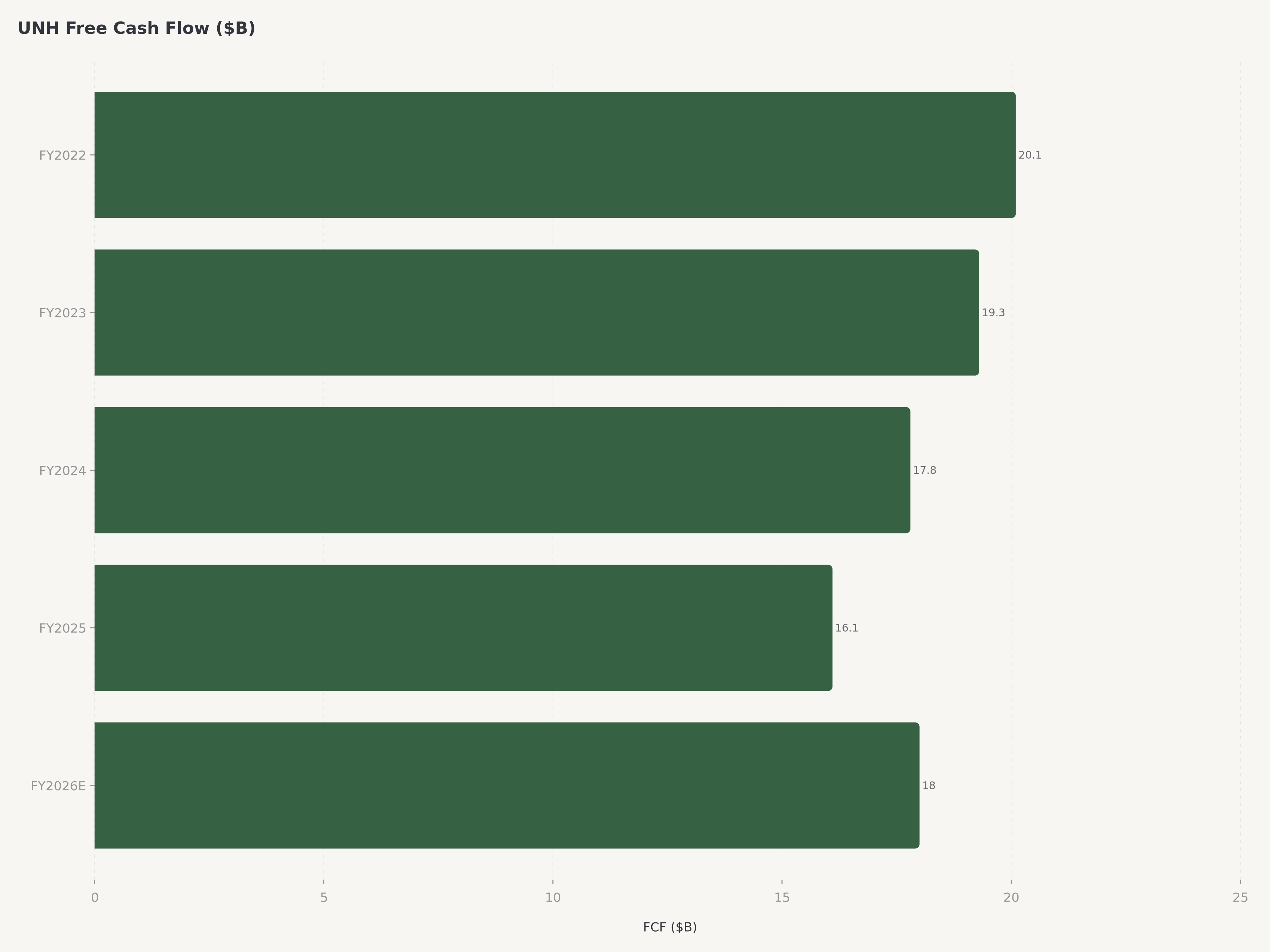
- Rentabilidad y flujo de caja: Un EPS GAAP de 21,11 $ y un EPS no-GAAP de 21,00 $ reflejan un poder de beneficios estable a pesar de una reducción estratégicamente deliberada de 2,8 millones de afiliaciones. La gerencia ha proyectado un flujo de caja libre de aproximadamente 18.000 millones de dólares para el año fiscal 2026, lo que respalda el dividendo trimestral de 2,21 $ por acción y la capacidad continua de retorno de capital.
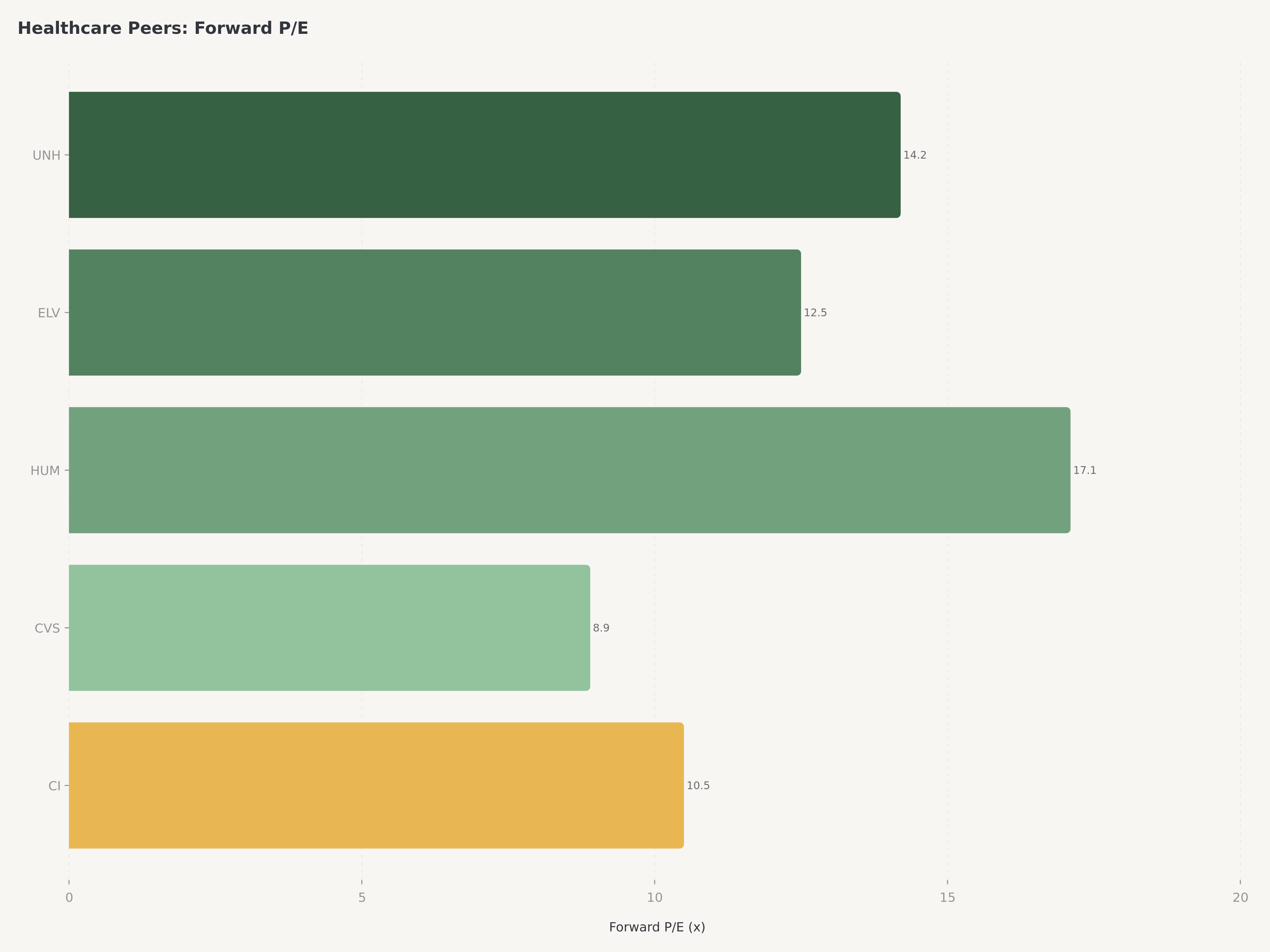
- Valoración y catalizador: Con un P/E proyectado de aproximadamente 14,2x, UNH cotiza con un descuento significativo respecto a su promedio de cinco años, a pesar de la mejora estructural de los márgenes en Optum. El informe de resultados del primer trimestre de 2026 publicado hoy (21 de abril) actúa como catalizador a corto plazo. Nuestro precio objetivo de 330 $ implica un potencial alcista de aproximadamente el 20%, respaldado por la trayectoria de crecimiento secular de Optum y una gestión disciplinada del Índice de Siniestralidad Médica (MLR).
Contexto macro: El panorama de la salud en EE. UU. en 2026
El sistema de salud de los Estados Unidos consume aproximadamente 4,8 billones de dólares anuales, lo que representa alrededor del 17,5 por ciento del producto interno bruto, una proporción que continúa su trayectoria ascendente de varias décadas impulsada por el envejecimiento de la población, la prevalencia de enfermedades crónicas y la innovación farmacéutica. Para las organizaciones de atención administrada, este crecimiento del gasto crea un viento de cola de ingresos duradero que pocos sectores pueden igualar. Los Centros de Servicios de Medicare y Medicaid proyectan un crecimiento del gasto nacional en salud del 5 al 6 por ciento anual hasta el final de la década, superando el crecimiento del PIB nominal y asegurando que el volumen subyacente de vidas aseguradas y transacciones médicas continúe expandiéndose.
El entorno político en 2026 presenta un panorama mixto. La inscripción en Medicare Advantage ha superado los 33 millones de beneficiarios, lo que representa más de la mitad de todas las personas elegibles para Medicare, una tasa de penetración que parecía aspiracional hace solo cinco años. Este cambio secular beneficia a los grandes operadores de atención administrada que pueden amortizar las inversiones en coordinación de la atención en grupos masivos de miembros. Sin embargo, el escrutinio regulatorio se ha intensificado. Los Centros de Servicios de Medicare y Medicaid finalizaron cambios en la metodología de ajuste de riesgo que reducen el beneficio de intensidad de codificación que los planes MA habían capturado históricamente, creando un viento en contra para el crecimiento de los ingresos por miembro que requiere disciplina operativa para compensar.
En el frente farmacéutico, las disposiciones de fijación de precios de medicamentos de la Ley de Reducción de la Inflación están remodelando la cadena de valor farmacéutica. El rediseño de Medicare Parte D, que limita los costos de bolsillo para los beneficiarios, traslada la responsabilidad financiera a los planes y a los administradores de beneficios farmacéuticos (PBM). Para los operadores integrados verticalmente como UnitedHealth Group, esto crea tanto un desafío como una oportunidad: el PBM debe absorber una mayor exposición a los costos, pero el modelo integrado permite una optimización interna entre seguros, farmacia y prestación de atención que los PBM independientes no pueden replicar.
El mercado laboral para los profesionales de la salud sigue siendo estructuralmente ajustado. La escasez de médicos, particularmente en atención primaria, ha acelerado el cambio hacia acuerdos de atención basados en el valor que compensan a los proveedores por los resultados en lugar del volumen. Esta transición juega directamente a favor de las fortalezas de las plataformas ricas en datos y habilitadas por tecnología, precisamente la capacidad que Optum ha pasado una década construyendo.
La transformación de UnitedHealth: De aseguradora a sistema de salud
La evolución de UnitedHealth Group durante la última década representa uno de los giros estratégicos más trascendentales en la historia corporativa estadounidense. Lo que comenzó como una compañía de seguros de salud tradicional se ha transformado en un conglomerado de servicios de salud integrado verticalmente que toca casi todos los elementos del ecosistema de prestación de atención y financiamiento. El arquitecto de esta transformación fue el difunto Andrew Witty, pero el plan estratégico perdura bajo Stephen Hemsley, quien regresó como CEO en mayo de 2025, trayendo de vuelta al ejecutivo que originalmente construyó la visión de Optum durante su mandato anterior de 2006 a 2017.
El regreso de Hemsley señala un énfasis renovado en la ejecución operativa y la disciplina de capital. Su primera gran decisión estratégica —la reducción deliberada de aproximadamente 2,8 millones de afiliaciones— inicialmente inquietó al mercado, pero revela una comprensión sofisticada de la economía de los seguros. Al salir de cohortes de miembros no rentables o marginalmente rentables, particularmente en ciertos contratos estatales de Medicaid y planes de intercambio individual con selección de riesgo adversa, UnitedHealth está priorizando la calidad del margen sobre el volumen de ingresos. Este es el libro de jugadas en el que Hemsley fue pionero en su primer mandato: crecer donde la economía unitaria es favorable, retirarse donde no lo es, y dejar que la plataforma Optum cree un valor que trascienda la suscripción de seguros.
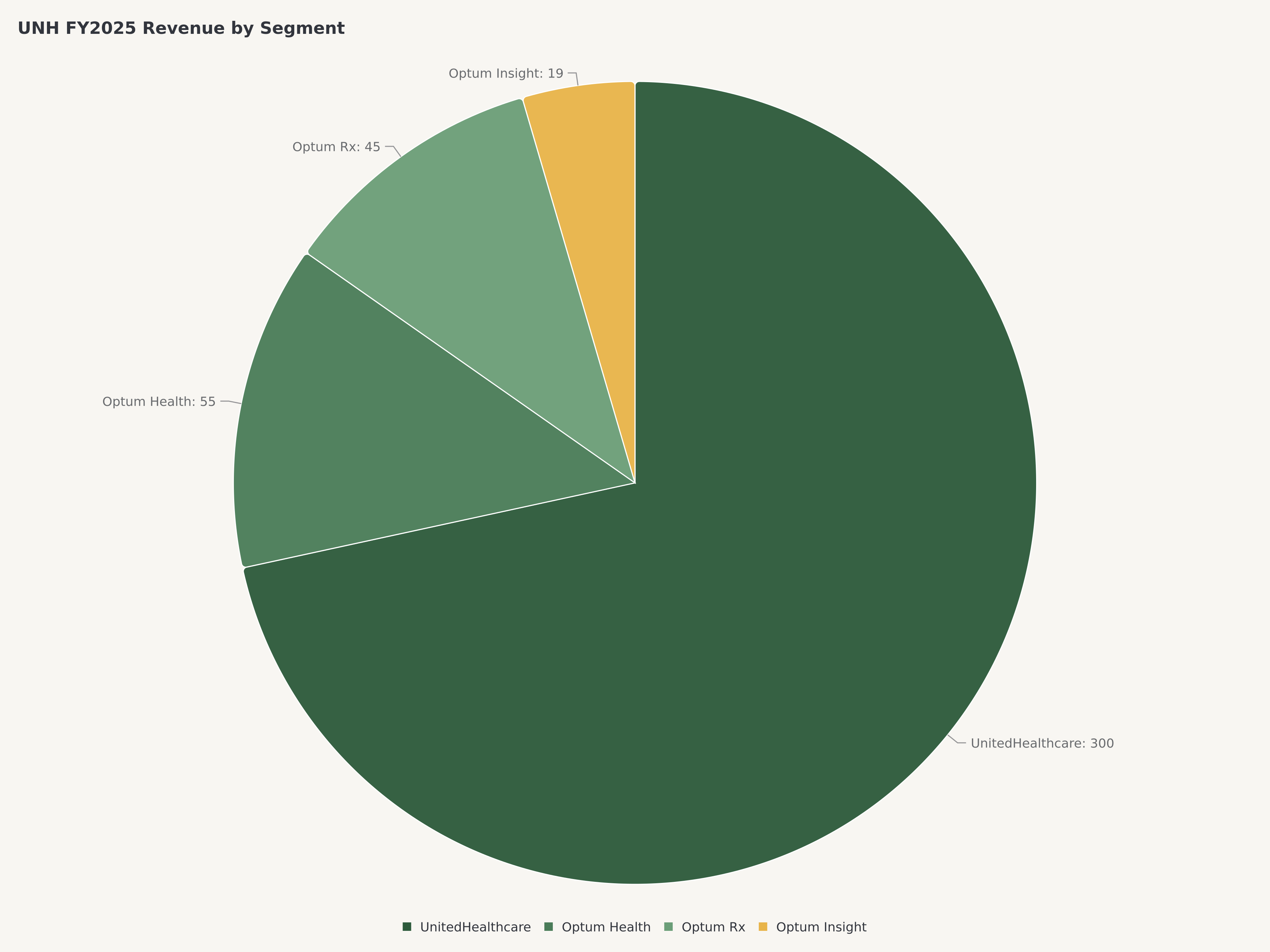
La estructura organizacional refleja esta identidad dual. UnitedHealthcare, la rama de seguros, proporciona la capa de distribución y acceso a los miembros, cubriendo aproximadamente 50 millones de miembros médicos a través de líneas de negocios patrocinadas por empleadores, individuales, Medicare Advantage y Medicaid. Optum, el conglomerado de servicios de salud, comprende tres plataformas interconectadas: Optum Health (prestación de atención y atención basada en el valor con más de 100.000 médicos alineados), Optum Insight (tecnología de salud, análisis y gestión del ciclo de ingresos) y Optum Rx (uno de los tres administradores de beneficios farmacéuticos más grandes del país, que procesa más de 1.400 millones de recetas ajustadas anualmente).
El genio estratégico reside en el efecto volante entre estas entidades. Los miembros de UnitedHealthcare reciben atención a través de los médicos de Optum Health, cuyos datos de resultados fluyen a través de la plataforma de análisis de Optum Insight, con recetas surtidas por la red de farmacias de Optum Rx. Cada transacción genera datos que mejoran la predicción de riesgos, los protocolos de atención y la gestión de costos, ventajas competitivas que se acumulan con el tiempo y son extraordinariamente difíciles de replicar para competidores menos integrados.
Desempeño operativo: El año fiscal 2025 ofrece escala y disciplina
Los resultados financieros del año fiscal 2025 de UnitedHealth Group demostraron la resiliencia de los beneficios del modelo integrado incluso durante un período de reequilibrio estratégico deliberado. Los ingresos totales de 419.300 millones de dólares representaron un aumento del 12 por ciento interanual, una tasa de crecimiento notable para una empresa que ya era el mayor generador de ingresos en el sector de la salud de EE. UU. Para contextualizar esta escala: los ingresos anuales de UNH superan el PIB de muchas naciones desarrolladas y son aproximadamente equivalentes a los ingresos totales de los cinco principales actores de la industria bancaria comercial de EE. UU. combinados.
Las ganancias por acción GAAP de 21,11 $ y el EPS no-GAAP de 21,00 $ reflejaron la estrecha brecha entre las ganancias reportadas y ajustadas que caracteriza a un negocio maduro y bien gestionado con distorsiones puntuales limitadas. La mínima divergencia entre GAAP y no-GAAP de aproximadamente 0,11 $ es en sí misma un indicador de calidad: sugiere que la gerencia no depende de ajustes agresivos para presentar una imagen de ganancias materialmente diferente de lo que requiere la contabilidad GAAP.
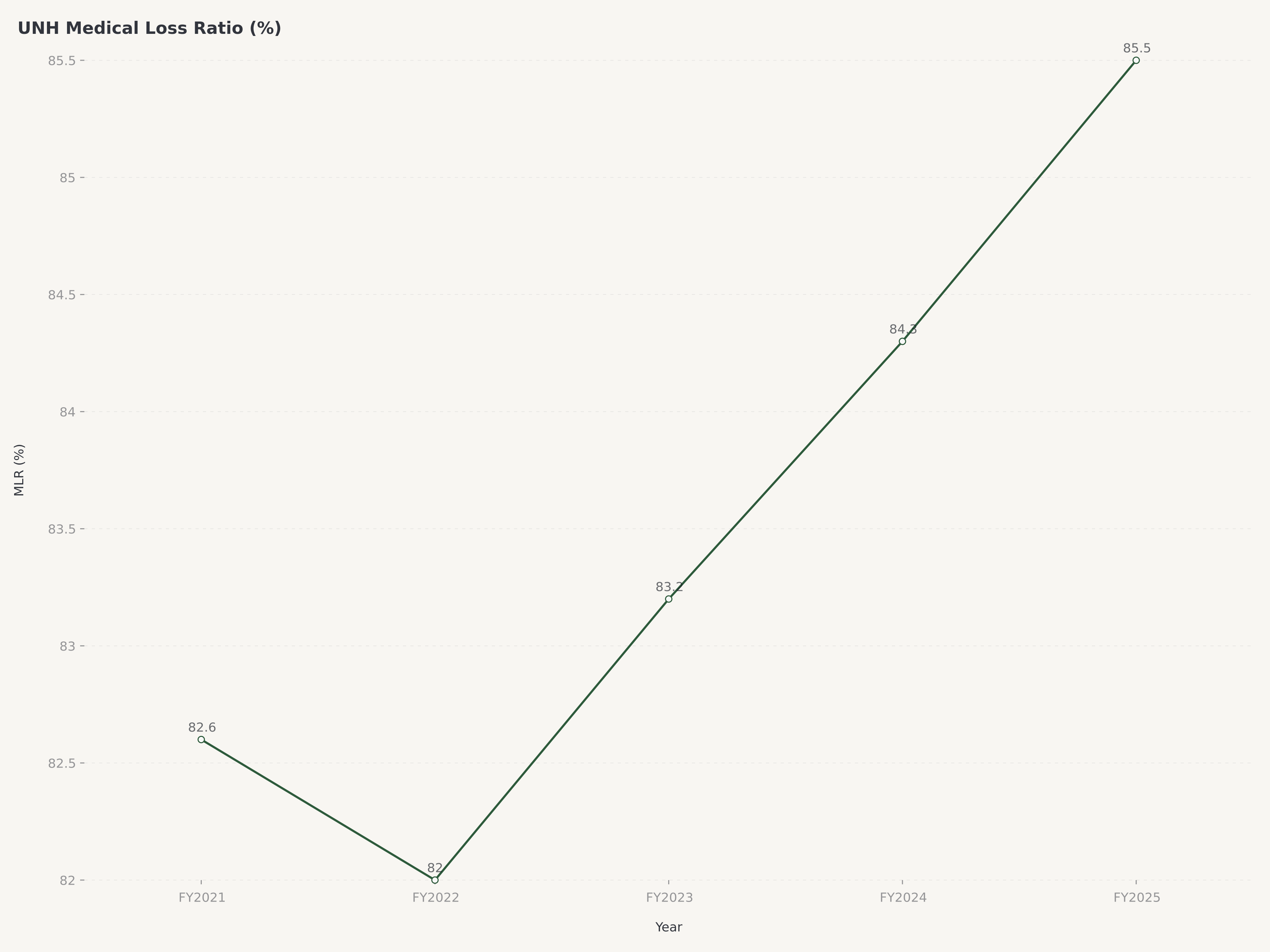
El Índice de Siniestralidad Médica —el porcentaje de los ingresos por primas gastado en reclamaciones médicas— sigue siendo la métrica operativa más importante para evaluar la rentabilidad de la atención administrada. Para las carteras comerciales y de Medicare Advantage de UnitedHealthcare, el MLR se ha gestionado dentro de un rango que equilibra los precios competitivos con la disciplina de suscripción. En un entorno donde las tendencias de costos médicos rondan el 6 al 7 por ciento (impulsadas por la normalización de la utilización pospandemia, la adopción de medicamentos GLP-1 y la demanda de salud conductual), mantener estable el MLR requiere una mejora operativa continua en la gestión de la atención, la contratación de redes y el diseño de beneficios. La reducción de 2,8 millones de miembros debería mejorar el MLR combinado en el futuro al eliminar las cohortes de mayor costo y menor margen.
Optum continuó superando la tasa de crecimiento consolidada. Optum Rx fue el más destacado, impulsado por la obtención de nuevos clientes, el volumen de farmacias especializadas y la integración de adquisiciones previas. El crecimiento de los ingresos en Optum Rx se benefició del cambio secular hacia los medicamentos especializados, que conllevan mayores ingresos por receta y donde la capacidad del PBM para negociar reembolsos con los fabricantes y gestionar la adherencia a la terapia crea un valor diferenciado. Optum Health amplió su huella de atención basada en el valor, agregando consultorios médicos y ampliando los acuerdos de asunción de riesgos con clientes pagadores (incluyendo, pero no limitado a, la propia UnitedHealthcare).
La asignación de capital reflejó la confianza de la gerencia en la trayectoria del negocio. El dividendo trimestral de 2,21 $ por acción —que representa un pago anualizado de aproximadamente 8,84 $— posiciona a UNH entre los pagadores de dividendos con crecimiento más confiable en el S&P 500. La compañía ha aumentado su dividendo durante 15 años consecutivos. La guía de flujo de caja libre de la gerencia de aproximadamente 18.000 millones de dólares para el año fiscal 2026 proporciona una capacidad amplia para el crecimiento continuo de dividendos, la recompra de acciones y adquisiciones complementarias en la prestación de atención y tecnología.
Inmersión profunda en salud: Optum y el Índice de Siniestralidad Médica
Optum: La plataforma que justifica la prima
La importancia de Optum para la tesis de inversión de UnitedHealth no puede exagerarse. Lo que comenzó como un centro de costos —una rama de tecnología y servicios que apoyaba a la aseguradora matriz— ha evolucionado hasta convertirse en un centro de beneficios independiente que se situaría como una empresa de la lista Fortune 25 de forma autónoma. Las tres ramas de la plataforma crean una posición competitiva que se refuerza a sí misma.
Optum Rx procesa más de 1.400 millones de recetas ajustadas anualmente, lo que lo convierte en uno de los tres PBM más grandes de los Estados Unidos junto con CVS Caremark y Express Scripts de Cigna. El negocio se beneficia de economías de escala masivas: cada receta incremental añade ingresos con una alta contribución marginal porque los costos fijos de gestión de formularios, contratación de redes de farmacias e infraestructura tecnológica ya están absorbidos. El giro estratégico hacia la farmacia especializada —donde la economía por receta es dramáticamente superior y donde las capacidades de gestión clínica diferencian— ha acelerado el crecimiento de los ingresos de Optum Rx hasta situarse entre los más rápidos de la empresa. A medida que los medicamentos agonistas del receptor de GLP-1 se expanden de la diabetes a la obesidad, la reducción del riesgo cardiovascular y potencialmente la enfermedad de Alzheimer, Optum Rx está posicionado para capturar una parte desproporcionada de la cadena de valor a través de la colocación en formularios, la gestión de autorizaciones previas y estructuras de reembolsos vinculadas a resultados.
Optum Health opera la red de prestación de atención ambulatoria más grande del país con más de 100.000 médicos alineados en atención primaria, atención de urgencia, centros quirúrgicos y salud conductual. El modelo de negocio está cambiando del pago por servicio a la capitación de riesgo total, donde Optum Health acepta un pago fijo mensual por miembro y es responsable de gestionar el costo total de la atención. Este modelo alinea los incentivos financieros con los resultados de salud y genera una economía superior cuando las capacidades clínicas y el análisis de datos permiten una mejor gestión de la salud de la población. La escasez de médicos crea una barrera estructural de entrada: adquirir e integrar consultorios médicos es intensivo en capital, depende de las relaciones y es operativamente complejo, todos ellos atributos que favorecen a un titular con la escala y el conocimiento institucional de Optum.
Optum Insight proporciona la capa de tecnología y análisis que une el ecosistema. El negocio sirve tanto a entidades internas de UnitedHealth como a clientes externos (hospitales, sistemas de salud, otros pagadores) con gestión del ciclo de ingresos, soporte de decisiones clínicas y análisis de salud de la población. Aunque es el segmento de Optum más pequeño por ingresos, Insight genera los márgenes más altos y produce la infraestructura de datos que hace que Optum Health y Optum Rx sean más efectivos. El negocio orientado al exterior también crea una dinámica competitiva sutil: los sistemas de salud que adoptan la tecnología de Optum Insight para sus propias operaciones pasan a formar parte del ecosistema de datos de UnitedHealth, profundizando los costos de cambio y creando ventajas de inteligencia que benefician la contratación de redes de UnitedHealthcare.
Índice de Siniestralidad Médica: La disciplina de gestión de márgenes
Para los inversores que evalúan a UnitedHealth Group, el Índice de Siniestralidad Médica es la métrica que conecta el crecimiento de los ingresos con la entrega de beneficios. Un aumento de un punto porcentual en el MLR en toda la base de primas de UNH se traduce en aproximadamente 2.500 a 3.000 millones de dólares en costos médicos incrementales, una cifra que ilustra tanto el apalancamiento inherente al modelo como la importancia existencial de la gestión del MLR.
El entorno actual de costos médicos presenta desafíos genuinos. La utilización pospandemia se ha normalizado y en algunas categorías ha superado los niveles anteriores a COVID, a medida que los procedimientos diferidos, las visitas de salud conductual y las pruebas de detección preventiva se aceleran. Los medicamentos GLP-1 representan una variable de MLR particularmente compleja: si bien ofrecen ahorros de costos reales a largo plazo a través de la gestión de la diabetes y la reducción de las comorbilidades relacionadas con el peso, su impacto a corto plazo en el gasto farmacéutico es sustancial, con costos anuales por paciente que superan los 10.000 $ para las formulaciones de marca.
La ventaja de UnitedHealth en la gestión del MLR proviene de su estructura integrada. Cuando los médicos de Optum Health gestionan las afecciones crónicas de forma proactiva, reducen los ingresos hospitalarios y las visitas a urgencias que generan la mayoría de los costos de las reclamaciones. Cuando Optum Rx negocia la colocación en formularios con los fabricantes farmacéuticos, puede orientar la prescripción hacia las terapias más rentables mientras comparte la economía de los reembolsos con los diseños de planes de UnitedHealthcare. Cuando los análisis de Optum Insight identifican a los miembros con un riesgo creciente de eventos médicos costosos, la infraestructura de coordinación de la atención puede intervenir antes de que los costos aumenten. Ningún competidor centrado puramente en seguros puede replicar esta optimización de circuito cerrado.
Valoración: El descuento respecto a la historia crea oportunidad
UnitedHealth Group cotiza a un P/E proyectado de aproximadamente 14,2x, un nivel que representa un descuento significativo respecto a su propio múltiplo promedio de cinco años de aproximadamente 18 a 20x. La capitalización de mercado de 245.000 millones de dólares, aunque enorme en términos absolutos, implica que el mercado está asignando un descuento de conglomerado a un negocio cuyos componentes individuales probablemente obtendrían valoraciones independientes más altas. Solo Optum, si se valorara con múltiplos de tecnología y servicios de salud comparables a sus pares, podría justificar una valoración cercana al valor empresarial actual de toda la compañía.
Nuestro precio objetivo de 330 $ se deriva de un marco ponderado por probabilidad de cuatro escenarios:
Caso alcista (20% de probabilidad): 400 $. Optum Rx captura una economía de la cadena de valor de GLP-1 superior a la esperada, el modelo de capitación de riesgo total de Optum Health ofrece una expansión de márgenes por encima de las expectativas, los resultados del primer trimestre de 2026 superan significativamente el consenso y el mercado vuelve a valorar a UNH hacia su P/E proyectado histórico de 18x. Este escenario requiere tanto un rendimiento operativo superior como una expansión de múltiplos, pero es alcanzable si la optimización de la afiliación de Hemsley ofrece una mejora visible del MLR en dos trimestres.
Caso base (50% de probabilidad): 330 $. Los ingresos crecen entre un 8 y un 10 por ciento en el año fiscal 2026, Optum mantiene su prima de crecimiento, el MLR se estabiliza dentro del rango guiado por la gerencia tras la reducción de la afiliación, y el P/E proyectado se revalúa modestamente de 14,2x hacia 16x a medida que se reconstruye la confianza de los inversores en la estrategia liderada por Hemsley. El FCF de aproximadamente 18.000 millones de dólares respalda el crecimiento continuo de dividendos y las recompras. Este escenario requiere una ejecución sólida sin suposiciones heroicas.
Caso de bajo rendimiento modesto (20% de probabilidad): 260 $. Las tendencias de costos médicos son más altas de lo esperado, los costos de los medicamentos GLP-1 crean una presión de MLR a corto plazo que tarda más en mitigarse y la reducción de la afiliación crea una desaceleración de los ingresos que el mercado penaliza al múltiplo deprimido actual. UNH cotiza lateralmente o ligeramente a la baja mientras los inversores esperan pruebas más claras de estabilización de márgenes.
Caso bajista (10% de probabilidad): 200 $. Una combinación de desarrollos regulatorios adversos (recortes agresivos de las tasas de Medicare Advantage, escrutinio antimonopolio de la integración vertical de Optum), una temporada de gripe severa o un resurgimiento de la pandemia que dispare la utilización, y una mayor incertidumbre sobre la transición del CEO crean un evento de rebaja de valoración material. Este escenario representaría una compresión de valoración históricamente extrema para UNH, pero es plausible en un entorno de riesgo de cola.
Precio objetivo ponderado por probabilidad: 20% x 400 $ + 50% x 330 $ + 20% x 260 $ + 10% x 200 $ = 80 $ + 165 $ + 52 $ + 20 $ = 317 $. Redondeamos a 330 $ para reflejar la opcionalidad alcista adicional de la economía de la plataforma de Optum y la probabilidad de que la disciplina operativa de Hemsley se manifieste en mejores tendencias de MLR antes de lo que supone el caso base.
Riesgos
El riesgo regulatorio y político representa la amenaza más material para la tesis de inversión. La integración vertical de UnitedHealth Group —particularmente la combinación de suscripción de seguros, prestación de atención y gestión de beneficios farmacéuticos bajo un mismo paraguas corporativo— ha atraído el escrutinio bipartidista de los legisladores que cuestionan si el modelo crea conflictos de intereses. La Comisión Federal de Comercio (FTC) ha aumentado su enfoque en la integración vertical de la salud, y cualquier acción legislativa o regulatoria que obligue a la separación estructural de Optum de UnitedHealthcare alteraría fundamentalmente el caso de inversión. La fijación de tarifas de Medicare Advantage por parte de CMS es un evento anual que introduce un riesgo binario en la economía por miembro, y la tendencia hacia coeficientes de ajuste de riesgo menos generosos es un viento en contra persistente.
La aceleración de la tendencia de los costos médicos representa una amenaza directa para las ganancias. Si bien la reducción de 2,8 millones de afiliaciones está diseñada para mejorar el perfil del MLR, el entorno subyacente de costos médicos se está intensificando. La utilización de medicamentos GLP-1 está creciendo a un ritmo que podría abrumar las negociaciones de reembolsos de los PBM, particularmente si nuevas indicaciones (riesgo cardiovascular, Alzheimer) reciben la aprobación de la FDA y generan una nueva ola de prescripciones. Una temporada severa de virus respiratorios, un evento pandémico inesperado o un aumento en los procedimientos quirúrgicos diferidos podrían elevar la utilización por encima de los supuestos actuariales incorporados en el precio de las primas. Para una empresa con la base de primas de UNH, cada 100 puntos básicos de deterioro del MLR se traduce en miles de millones de dólares en compresión de márgenes.
El riesgo de ejecución de la transición del CEO merece atención. El regreso de Stephen Hemsley fue generalmente bien recibido por los inversores de UNH a largo plazo que le atribuyen la construcción de la plataforma Optum, pero cualquier transición de liderazgo introduce incertidumbre sobre las prioridades estratégicas, la filosofía de asignación de capital y la cultura organizacional. La decisión de reducción de afiliaciones —tomada a los pocos meses del regreso de Hemsley— fue un movimiento audaz que tardará varios trimestres en validarse a través de los resultados financieros. Si la estrategia no produce una mejora visible del MLR para mediados del año fiscal 2026, la paciencia de los inversores podría erosionarse.
La competencia y la desintermediación representan riesgos estructurales a más largo plazo. La continua expansión de Amazon en farmacia y atención primaria (a través de One Medical y Amazon Pharmacy), combinada con participantes nativos tecnológicos que aplican inteligencia artificial a la coordinación de la atención y el procesamiento de reclamaciones, podría erosionar las ventajas competitivas de Optum en un horizonte de varios años. Si bien la escala y el foso de datos de UNH proporcionan un aislamiento sustancial, el panorama de la tecnología de la salud está evolucionando rápidamente y la veteranía por sí sola no garantiza un posicionamiento competitivo sostenido.
Conclusión
UnitedHealth Group a 275,60 $ representa una oportunidad poco común de adquirir la franquicia más formidable de la salud en EE. UU. con un descuento de valoración que no refleja las ventajas competitivas estructurales de la compañía. El regreso de Stephen Hemsley y su enfoque inmediato en la calidad del margen sobre el volumen de afiliaciones señalan un equipo de gestión que entiende la diferencia entre crecimiento y creación de valor. La plataforma Optum —particularmente el posicionamiento de Optum Rx en el centro de la revolución farmacéutica de los GLP-1 y la expansión de la prestación de atención basada en el valor de Optum Health— proporciona vectores de crecimiento secular que son en gran medida independientes de los ciclos de suscripción de seguros. Con un P/E proyectado de 14,2x frente a un flujo de caja libre guiado de aproximadamente 18.000 millones de dólares, el perfil de riesgo-recompensa favorece a los inversores pacientes. Calificamos a UNH como Compra con un precio objetivo de 330 $.
Para los lectores interesados en temas intersectoriales relacionados, nuestro análisis de la transformación del aluminio de Alcoa ilustra cómo los giros estratégicos en las industrias tradicionales pueden desbloquear el valor para los accionistas, mientras que nuestra cobertura del modelo de crecimiento impulsado por la publicidad de Netflix explora la economía de las plataformas y la dinámica de expansión de márgenes en un contexto sectorial diferente.
Preguntas frecuentes
¿Qué hace UnitedHealth Group y cómo gana dinero?
UnitedHealth Group opera a través de dos plataformas de negocios principales. UnitedHealthcare es uno de los mayores proveedores de seguros de salud en los Estados Unidos, cubriendo aproximadamente 50 millones de miembros médicos a través de planes patrocinados por empleadores, individuales, Medicare Advantage y Medicaid. Obtiene ingresos por primas y gestiona los costos médicos a través de la contratación de redes, la gestión de la atención y el diseño de beneficios. Optum es una plataforma diversificada de servicios de salud, tecnología y gestión de beneficios farmacéuticos que comprende Optum Health (prestación de atención con más de 100.000 médicos alineados), Optum Insight (tecnología y análisis de salud) y Optum Rx (beneficios farmacéuticos que procesan más de 1.400 millones de recetas ajustadas anualmente). Juntos, estos negocios generaron 419.300 millones de dólares en ingresos en el año fiscal 2025.
¿Qué es el Índice de Siniestralidad Médica y por qué es importante?
El Índice de Siniestralidad Médica es el porcentaje de los ingresos por primas que una aseguradora de salud gasta en reclamaciones médicas y actividades de mejora de la calidad. Es la métrica de rentabilidad más importante para las compañías de atención administrada porque determina cuánto de cada dólar de prima se retiene como margen bruto para gastos operativos y beneficios. Bajo la Ley de Cuidado de Salud a Bajo Precio, las aseguradoras deben mantener MLR mínimos (80% para individuos y grupos pequeños, 85% para grupos grandes), pero el objetivo operativo es gestionar el MLR lo más cerca posible de estos mínimos manteniendo precios competitivos y el cumplimiento regulatorio. Para UnitedHealth Group, cada punto porcentual de mejora del MLR en toda su base de primas representa aproximadamente entre 2.500 y 3.000 millones de dólares de beneficio en ganancias.
¿Por qué UnitedHealth redujo 2,8 millones de afiliaciones?
La reducción de afiliaciones fue una decisión estratégica deliberada del CEO Stephen Hemsley a su regreso para mejorar la calidad de la cartera de seguros de UnitedHealthcare. Al salir de aproximadamente 2,8 millones de afiliaciones concentradas en cohortes no rentables o marginalmente rentables —particularmente ciertos contratos estatales de Medicaid y planes de intercambio individual con selección de riesgo adversa— la compañía busca mejorar su Índice de Siniestralidad Médica combinado y la calidad general de los beneficios. Si bien la decisión redujo temporalmente la escala de ingresos, refleja una comprensión sofisticada de que no todos los miembros contribuyen por igual a la rentabilidad, y que una base de miembros más pequeña y rentable puede generar retornos superiores para los accionistas.
¿Cómo se compara Optum con sus competidores?
Optum compite en múltiples subsectores de la salud. En la gestión de beneficios farmacéuticos, Optum Rx rivaliza con CVS Caremark y Express Scripts de Cigna como uno de los tres PBM más grandes. En la prestación de atención, Optum Health es la red de médicos ambulatorios más grande del país, compitiendo contra grupos de médicos empleados por sistemas de salud y plataformas respaldadas por capital privado. En tecnología de la salud, Optum Insight compite con proveedores especializados en gestión del ciclo de ingresos, análisis y soporte de decisiones clínicas. Lo que diferencia a Optum es la integración vertical de los tres dominios bajo el paraguas de UnitedHealth Group, creando ventajas en el intercambio de datos y la coordinación de la atención que los competidores aislados no pueden replicar.
¿Cuál es la perspectiva de dividendos y retorno de capital de UnitedHealth Group?
UnitedHealth Group paga un dividendo trimestral de 2,21 $ por acción, lo que representa un pago anualizado de aproximadamente 8,84 $ por acción. La compañía ha aumentado su dividendo durante 15 años consecutivos, estableciendo uno de los historiales de crecimiento de dividendos más consistentes en el S&P 500. Con la gerencia proyectando un flujo de caja libre de aproximadamente 18.000 millones de dólares para el año fiscal 2026, el dividendo consume solo una modesta porción de la generación de efectivo, dejando una capacidad sustancial para recompras de acciones y adquisiciones estratégicas. La combinación de un P/E proyectado de 14,2x, una capitalización de mercado de 245.000 millones de dólares y 18.000 millones de dólares en generación anual de flujo de caja libre crea un perfil de retorno total atractivo compuesto por ingresos de dividendos más el potencial de apreciación de capital.
Descargo de responsabilidad: Este artículo es solo para fines informativos y no constituye asesoramiento de inversión, una solicitud o una recomendación para comprar, vender o mantener ningún valor. Las opiniones expresadas son las del autor y no reflejan necesariamente las de Edgen.tech. Invertir implica riesgos, incluida la posible pérdida del capital. El rendimiento pasado no es indicativo de resultados futuros. Las inversiones en salud están sujetas a riesgos regulatorios, políticos y clínicos. Los lectores deben realizar su propia investigación y consultar a un asesor financiero calificado antes de tomar decisiones de inversión. Edgen.tech y sus analistas pueden mantener posiciones en los valores discutidos aquí.
Invertir, por fin, ya no es cosa de uno solo.
Prueba Ed gratis. Sin tarjeta, sin compromiso.